Anorexia & Food Restriction EXPLAINED (Adapted to Flee Famine Hypothesis PART 4)
Mar 28, 2022
Welcome to part 4 of my 7-part series on the Adapted to Flee Famine Hypothesis, a scientific and revolutionary explanation of Anorexia Nervosa! So far, you’ve learned about 4 current theories being used to understand Anorexia, why they lack conclusiveness, and how the Adapted to Flee Famine Theory provides an alternative view of the illness. Now, it’s time to look at the three core adaptations of anorexia as proposed by the AFFH, which are restriction, hyperactivity, and denial of starvation. In this post, we’re going to be focusing on restriction!
Restriction
Food restriction is one of the three core symptoms of Anorexia. Whereas the theories mentioned in part 2 of this series hypothesize food restriction to be a deliberate act of control or rebellion, the paradoxical behavior has also been observed in animal studies.
Animal Studies
When rats are starved in a lab and are given access to a running wheel, they will eventually refuse their food completely and run themselves to death. Some breeds of pigs can develop “wasting pig syndrome” where they will start to pace incessantly and ignore their food when they lose additional weight. We will get deeper into the compulsive movement piece in part 5, but I just want to note something here, now that we have clear evidence of food refusal in species other than humans: would we ask the rats or pigs refusing food if they felt sad or lonely, or blame their insufficient intake on childhood trauma? Not to mention, we wouldn’t blame their food refusal on fear of fatness either!

Anorexia during the Middle Ages
Not being able to associate fear of fatness with food refusal is also illustrated in the earliest recorded accounts of Anorexia. During the Middle Ages, a time when many religious women fasted, some developed “holy anorexia”. The Roman Catholic Church officially canonized over 85 very thin saints, blesseds, or venerables who were recognized, in part, for their seemingly miraculous ability to live with little food.

Diaries and other first-hand accounts show that these women manifested typical AN symptoms of aversion to food, overactivity, and denial of starvation, even though they lived in a time period where the ideal female body was not an underweight one.
Anorexia in Wild Animals
Aside from controlled animal studies and historic accounts, appetite also appears to be suppressed in wild animals when hunger and feeding compete with seemingly more important activities. When they need to defend their territory, incubate, or migrate, several species will stop eating, even if food is readily available. As a result, body weight may drop considerably and the animals continue to restrict food, as stopping to “eat and run” would interfere with migration.
Anorexia and the Neuroendocrine System
Another consistent trait across humans and other mammals who display symptoms of anorexia, can be found in the neuroendocrine system. In my course Extremely Hungry to Completely Satisfied, I explain in depth how hunger and satiety cues are regulated in the body, so I recommend you enroll to gain a deeper understanding of those signals and of course, what I’m about to explain with regards to the signals in anorexia!
Normally, when an individual begins to starve, neurochemical signals of hunger are elevated and signals for satiety and activity are lowered. However, Anorexia researchers have found that most neuromodulators and hormones influencing hunger, satiety, and activity are present in unusual concentrations that are opposite to those found in “normal” starvation.
These findings are all consistent with adaptations to turn off eating and turn on traveling, as well as most anorexic’s descriptions of finding it very difficult to eat and feeling restless and driven to exercise.
Hunger & Fullness
I remember during my own eating disorder, I found it difficult to eat simply because I felt full very quickly. As I describe in my course, fullness is signaled to the brain by fat cells. Researchers have found that leptin levels elevate more rapidly than weight gain in individuals recovering from anorexia, which helps to understand why it’s so hard to eat more in the early stages of recovery, even though your body so desperately needs the food.
This is why it’s SO important to honor mental hunger (which is a form of Extreme Hunger!), because your body may physically be unable to communicate the extreme hunger with you! That is why it will opt for a more energetically efficient way to communicate hunger with you, which is THINKING about food!
Furthermore, leptin levels often remain elevated in recovered anorexics. These findings led researchers to conclude that anorectics’ low body weight appears to be physiologically defended and helps explain why most people who develop anorexia have naturally lower setpoints.
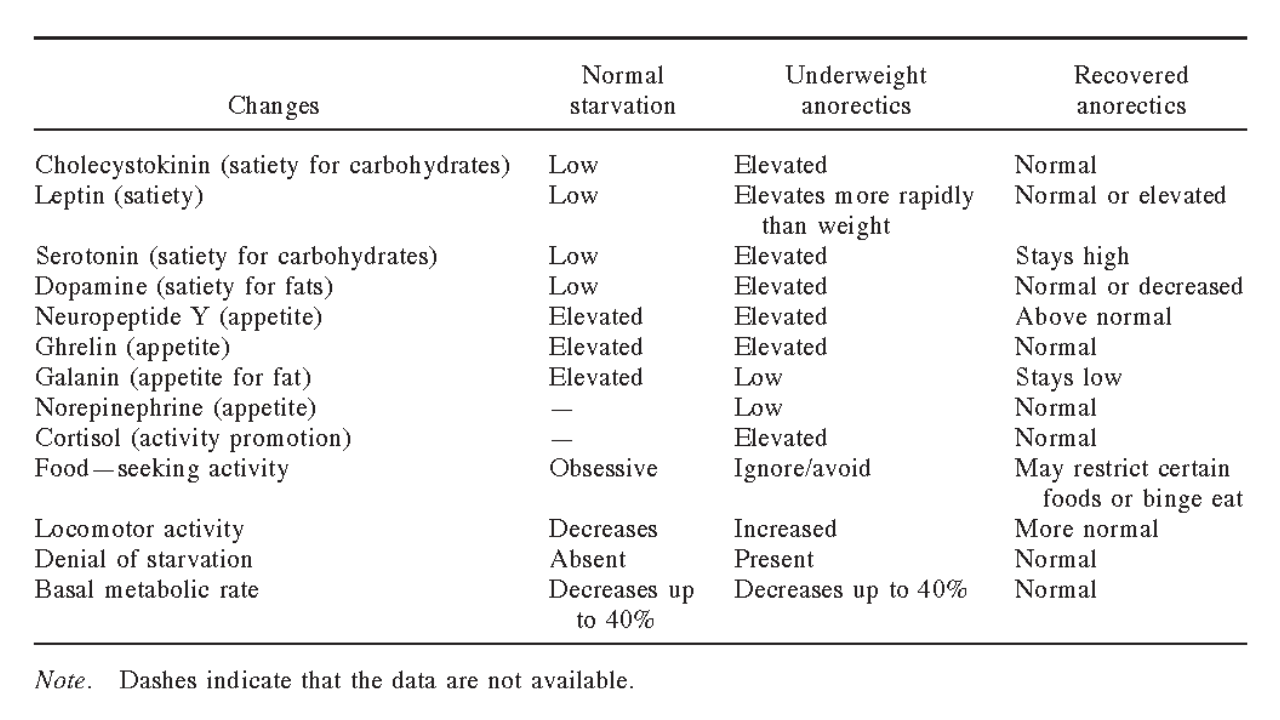
Table shows behavioral, cognitive, physiological, and neuroendocrine changes exhibited in normal starvation, underweight anorectics, and recovered anorectics
Other hormones that contribute to early satiety are cholecystokinin, serotonin, and dopamine. Cholecystokinin and serotonin specifically, are responsible for satiety of carbohydrates, while dopamine is responsible for satiety of fats. These satiety hormones are elevated in underweight anorexics, and often remain elevated even in recovered individuals. What’s more, is that elevated levels of serotonin have been linked to traits of perfectionism and rigidity, commonly observed in individuals with anorexia.
Interestingly, the appetite-promoting hormone galanin stays low in recovered anorexics. Abnormally low levels of galanin, a neuropeptide that stimulates appetite for fat, could potentially aid in understanding the aversion to high-fat foods not only in people with active anorexia, but even after they have been weight restored.
Genetic Mutations
Researchers are still closing in on the genetic mutations that lead to some of the biochemical alterations of appetite and satiety in AN. Leptin, melanocortin receptors and their antagonists are responsible for the precise regulation of fat stores, and an individual’s unique levels will defend their set point weight.
In some forms obesity, mutations that lead to loss of function in these molecules have been found, resulting in lack of satiety and thus, stimulating overeating.
In a 2001 study, researchers found that a large percentage of Anorexia patients carried the same genetic mutation on a melanocortin antagonist, meaning the same gene functions opposite to the way in which it functions in a person who is genetically predisposed to be obese. This genetic finding explicates why anorexia sufferers with the genetic mutation are prone to abnormally early satiety, even when they are drastically underweight.
Stress & Reward Systems
Hormones involved in stress & reward systems may also contribute to the paradoxical feelings of virtuousness when food is restricted. Although it is atypical, stress-seeking behavior has been described in several mammalian species, including humans. One study suggested that a mechanism for the development of AN may be the reward that some individuals experience from stress, which would support the adaptation to flee famine.
Reward is meditated by the firing of dopamine neurons in the brain and enhanced by the secretion of adrenal hormones. Corticosterone is a specific adrenal hormone involved in the regulation of energy, immune reactions, and stress responses. It can stimulate feelings of euphoria and hyperactivity, which is fascinating considering the fact that increased levels of this hormone have been found in underweight anorexics!
In conclusion, the stress of overexercise and extreme dieting may activate reward mechanisms in the brain, so that self-starvation is initially rewarding and subsequently conditioned. In a time of famine in which migration would have been a top priority, such an inverted reaction to a stressful situation would have been lifesaving.
Appetite and Food Obsession
In contrast to biochemical alterations that promote satiety, neuropeptide Y and ghrelin, potent appetite-stimulating molecules, are elevated in underweight anorexics. This elevation may be responsible for the obsession with food, which often manifests as a sudden and fanatic interest in recipes and cooking. Because of the biochemical changes discussed earlier, anorexic individuals will still refuse food despite their obsession for it.
This too, is consistent with the adapted to flee famine theory. Why else would a powerful appetite-stimulating signaler remain high in AN if the function of the other changes was to postpone food searches until migration was completed? Presumably, if there were no hunger signaling mechanisms whatsoever (so no mental hunger), prehistoric people with AN would not have begun eating when they arrived in the lands of abundance.
Conclusion
You’ve made it to the end of part 4, all about how restriction is an adaptive mechanism to facilitate fleeing a famine! If you want to get even MORE value and achieve full recovery backed by SCIENCE, enroll in my course or learn more about 1-1 coaching!
FULL TEXT: Adapted to Flee Famine Hypothesis




